Systemic Microbiology
Antimicrobials
Bacterial Genetics
Blood and CSF
Eye and Ear
Genital Tract
Gastrointestinal Tract
Heart
Respiratory Tract
Urinary Tract
Antimicrobials
Definitions:
● Selective toxicity -- hurts the bug and not the host
● Bacteriostatic - inhibits bacterial growth (Chloramphenicol, Erythromycin & other macrolides
Clindamycin, Sulfonamides, Trimethoprim, Tetracycline, Linezolid, Quinupristin / dalfopristin)
-- Bactericidal - directly kills bacteria
(Aminoglycosides, Β-lactams, Vancomycin, Daptomycin, Teicoplanin, Telavancin , Quinolones (ie. Ciprofloxacin, levofloxacin), Rifampin, Metronidazole)
● Chemotherapeutic agent - abx to treat infx
● Antimicrobial agent - anything that stops or kills bug
● Antibiotic - rx made by bacteria / fungi
● Mechanism of Action - how the rx works
● Spectrum of activity - spectrum of bugs killed by rx
Requirements for ANTIMICROBIAL ACTIVITY
1. Agent must be in active form
2. Active drug must contact the target organism
3. Intracellular uptake
4. Target binding
5. Growth inhibition --> Lysis and death
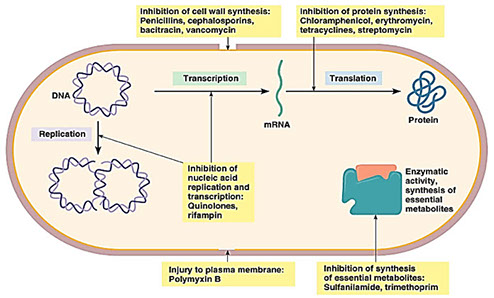
Modes of Action
A. Antibiotics affecting cell wall synthesis
B. Agents affecting the cell membrane
C. Inhibitors of protein synthesis
D. Antibiotics interfering with nucleic acid function
E. Metabolic antagonism
ANTIBIOTICS AFFECTING THE CELL WALL
OVERVIEW OF CELL WALL SYNTHESIS
● Cell wall synthesis occurs in three stages:
1. First stage - in the cytoplasm synthesizes cw building blocks (N-acetyl glucosamine / N-acetylmuramic acid [NAG and NAM])
2. Second stage - in cell membrane, NAMA is transferred to a membrane-bound lipid & then NAG added
3. Third stage - exterior to the cell membrane cross- linking of parallel peptidoglycan chains (aka the transpeptidation reaction)
● C.w. synthesis catalyzed by specific enzymes (transpeptidases, carboxypeptidases, endopeptidases)
● These regulatory proteins are referred to as penicillin binding proteins (PBPs)
β-LACTAM ANTIMICROBIAL AGENTS
Mechanism: actively growing bacteria gets PBPs bound in the cell membrane which inhibits peptidoglycan synth
Resistance mechanisms
● β-lactamases enzymes made by bacterium that inactivate β-lactam antibiotics by cleaving the β-lactam ring
● Low-affinity PBPs
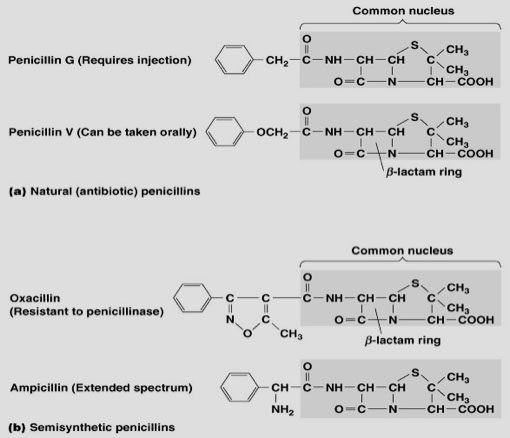
PENICILLINS
● Natural penicillins (penicillin G and Penicillin V)
● Pen G (parenteral) is most useful and widely used
-- pen V is oral
--good against S pneumo, strep pyogenes, viridans, and anaerobic gram + cocci
● Penicillinase-resistant penicillins have chemically altered side chains and include Methicillin, Oxacillin, Nafcillin
● Extended-spectrum penicillins - Carbenicillin, Ticarcillin, Piperacillin
● β-lactamase inhibitors - bind β-lactamases and inhibits inactivation of the penicillin antibiotic
OTHER β-LACTAMS
Cephems - includes cephalosporins which have a fused β-lactam ring not as susceptible to hydrolysis by penicillinase
Carbapenems - resistant to many β-lactamases (Imipenem)
- carbapenem-resistant Enterobacteriaceae (CRE) in healthcare news in 2015 (UCLA, traced to EDG, 1/2 die if systemic)
-- CRE aka Kleb pneumoniae carbapenemase / KPC or New Delhi Metallo-beta-lactamase / NDM
Monolactams --> Aztreonam
Cycloserine
Bacitracin - used topically in combo c Polymyxin B and / or Neomycin
- Vancomycin - very complex molecular structure (a disaccharide linked to three aromatic rings)
● Glycopeptide that binds to precursors of c.w. synthesis rather than attack PBPs
-- Teicoplanin - another glycopeptide
ABx AFFECTING CELL MEMBRANE
POLYMYXINS
● Five types, usually used topically in combination with bacitracin and neomycin
● Bind specifically to the outer membrane disrupting phospholipid & LPS
● Toxicity is a problem
● Polymyxin B
● Polymyxin E (Colistin)
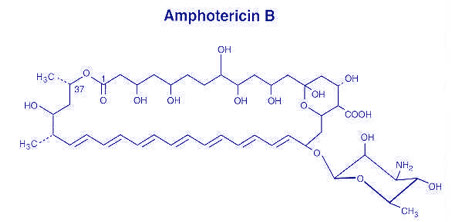
POLYENES
● Selectively inhibit organisms with sterols in their membranes (fungi and other eukaryotic microorganisms)
- Amphoteracin B
● Active against most fungi causing deep-seated mycoses
● Nephrotoxicity is a problem
● Conerstone of antifungal therapy
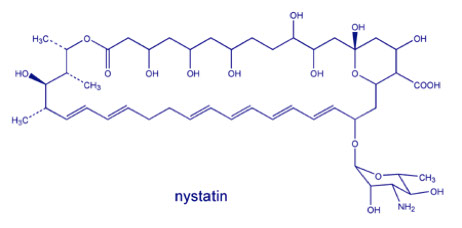
- Nystatin
● Antifungal used in treatment of superficial infections especially those
caused by Candida
● Used topically so toxicity is not a problem
PROTEIN SYNTHESIS INHIBITORS
INHIBITORS OF TRANSCRIPTION
- Actinomycin - valuable research tool but toxicity prevents it’s use clinically
- Rifamycins
● Ansa compounds aromatic ring spanned by a long aliphatic bridge
-- Rifampicin - most useful member of the group
● Used in the oral treatment of TB almost always in combination with other drugs (due to problems with resistance)
TRANSLATION INHIBITORS
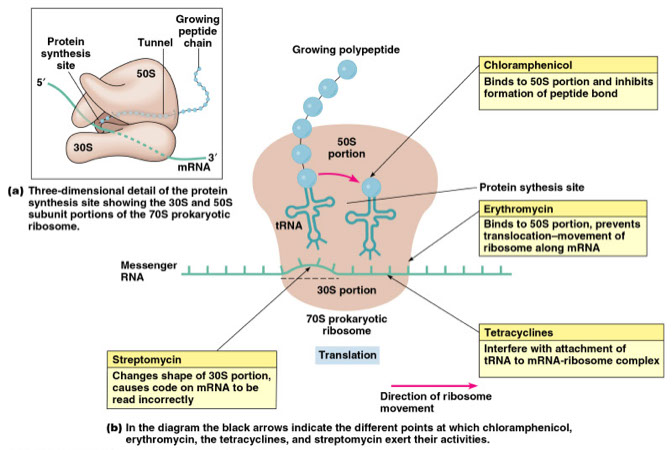
Inhibitors of the 30s ribosomal subunit
a) Aminoglycosides
● Streptomycin - usefulness limited 2/2 resistance
and newer aminoglycosides with broader spectrum of activity
● Other aminoglycosides: Neomycin, Kanamycin, Gentamicin, Tobramycin, Amikacin, Spectinomycin,
● Most are bactericidal and cause misreading of the mRNA
b) Tetracyclines
● Over use has resulted in a high level of resistance
● Tx Chlamydia & rickettsia infx, UTI
c) Nitrofurans
● Nitrofurantoin - synthetic bactericidal, tx UTIs
Inhibitors of the 50s ribosomal subunit
a) Chloramphenicol - broad-spectrum, bacteriostatic
● Anaerobic infections, Haemophilus meningitis, typhoid fever
● Somewhat toxic
b) Macrolides
● Contain a lactone ring
● Erythromycin - Spectrum similar to penicillin (useful in treating patients allergic to penicillin)
● Mycoplasma pneumoniae, Legionnaires disease,
Campylobacter enteritis are all treated with Erythromycin (D of C)
- Other 50s inhibitors: Lincomycin and Clindamycin,
Puromycin and Fusidic Acid
- Aminoacyl-tRNA synthetase enzymes play crucial role in protein biosynthesis, which can be inhibited by Mupirocin (inactivates bacterial isoleucyl-tRNA synthetase) and are used in MRSA infx
DNA FUNCTION INTERFERERS
Mitomycin: Important research tool, not useful clinically
Nalidixic Acid:
● Inhibits DNA gyrase activity
● Urinary tract infections caused by Gram negatives
Novobiocin
● Used to treat infections caused by Penicillin resistant Staphylococcus
Griseofulvin
● Specific for fungi with cell walls of chitin
● Used to treat ringworm infections that fail to respond to topical therapy
● Prolonged oral administration
Actinomycin & Rifamycins (Transcription inhibitors)
METABOLIC OR COMPETITIVE ANTAGONISM
● Enzymes are inhibited by compounds possessing a structure similar to the
natural substrate.
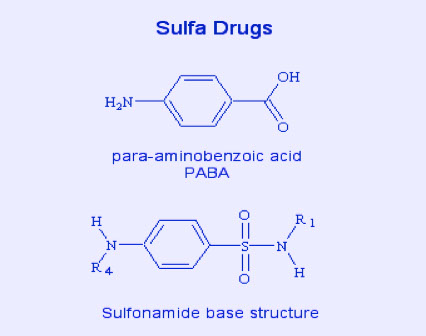
Sulfonamides
● Derivatives of ρ-aminobenzenesulfonamide
● Wide spectrum of activity
● Structure of PABA is similar to that of sulfanilamide
(competitive inhibition)
-- folic acid cant cross bacterial cell wall (can cross human cell wall), so needs to be made from PABA
--- folic acid synth has 2 rxns, when sulfa used the first rxn makes pteridine and sulfa drug, and the 2nd rxn that makes PABA and glutamic acid inhibited
● Used against S. pyogenes, S. pneumoniae, H. influenzae, cholera, plague, Chlamydia, N. meningitis, and other infectious agents
● Side effects - renal blockage, allergic rxns, etc.
Sulfones
● Dapsone
● Analog of PABA (leprosy)
Para-Aminosalicylic Acid
● Analog of PABA
● Second line drug in the treatment of TB
Trimethoprim/Sulfamethoxazole
● Antifolic compound used in combination with sulfamethoxazole
- TMP binds DHF reductase and inhibits reduction to THF, an essential precursor in thymidine sunth pathway and thus inhibiting bacterial DNA synth
● UTI, Salmonella, chronic bronchitis
● Active against both Gram negatives & Gram positives (parasites also)
Isoniazid
● Highly specific for TB
● Effective in very low concentration
● Bactericidal only for actively growing cells
● Given in combination with ethambutol or streptomycin (the mainstay of treatment for TB)
Bacterial Genetics
Transformation - take up DNA from envt
- aka "competence"
- feature of the SHiN bacteria
Conjugation
- plasmid xchange, not chromosomal DNA
- types: F+ x F- or Hfr x F-
- F+ x F- : F+ plasmid has genes reqd for conjugation, bacteria w/o the plasmid (called "F-"); F+ send F- plasmid DNA through pilus (no chromosomal DNA sent)
- Hfr x F- : F+ plasmid incorporated to bacterial chromosomal DNA (Hfr cell); plasmid and chromosomal genes transferred
Generalized transduction - "Packing" process
- lytic phages infcts bacteria causing cleavage of bacterial DNA and synth of viral proteins
- sections of chromosomal DNA from bacteria can get put in viral capsid; phage infx another bacteria, spreading the gene
Specialized transduction - "Excision" event
- lysogenic phages infx bacteria, taken up by bacterial chromosome, and genes flanking can be excised
- then can go on to infct another bacteria
Transposition - DNA that "jumps" (excised and reincorporated)
- transfers genes from plasmid to chromosomal DNA and back, and can catch some flanking bacterial DNA
Spectrum of Activity

Basic req's for abx to work and places it can be blocked (X)
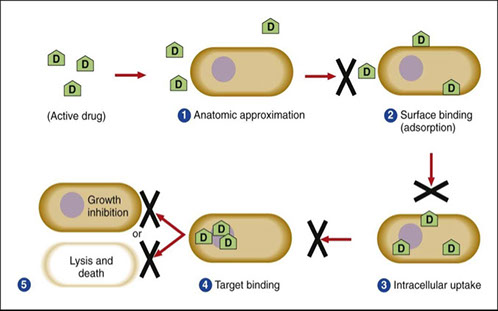
Abx modes of action

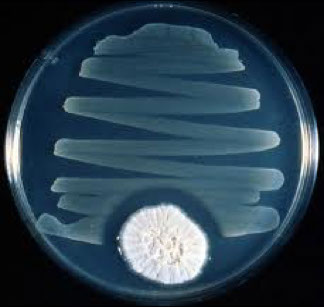
Penicillum spp



Vancomycin



Novobiocin


Blood and CSF Infections
BACTEREMIA - bacteria in the blood
1. Transient:
- Manipulation of infected tissues
- Instrumentation of contaminated mucosal surfaces
- Surgery in contaminated areas
- Occurs early in the course of many systemic and localized infections
2. Intermittent:
- Most often associated with undrained abscesses
- Abscesses are common cause of FUO
3. Continuous:
- Feature of acute and subacute bacterial endocarditis as well as other intravascular
infections
- Also occurs during first few weeks of typhoid fever and Brucellosis
SOURCES OF BACTEREMIA
25% G.U. Tract 5% Surgical Wounds
20% Respiratory Tract 10% Other Known Sites
10% Abcesses 25% Uncertain Sites
5% Biliary Tract
COMMONLY ISOLATED BACTERIAL SPECIES CAUSING BACTEREMIA
Gram Negatives
- usually Enterobacteriaceae and Pseudomonadaceae
- Bacteremias caused by other Gram negatives are considered to be discrete clinical entities
- Frequency of occurance: E. coli, KES group, Ps. aeruginosa, Proteus spp., Bacteroides spp., other Gram negatives
Gram Positives
- Most common isolate is Staphylococcus epidermidis
- Most of these isolates are "contaminants"
- Frequency of occurance: S. aureus, Str. pneumoniae, Enterococci, Gp. A Strep, other
Streptococcus spp., Gp. B Strep, anaerobic cocci, Cl. perfringens, Corynebacterium spp., Listeria spp.
OTHER RELEVANT ORGANISMS ISOLATED FROM BLOOD
- HACEK Bacteria: Organisms include Haemophilus aphrophilus, Actinobacillus actinomycetemcomitans, Cardiobacterium hominis, Eikenella corrodens, Kingella kingae
- Other Fastidious Bacteria: Campylobacter spp., Capnocytophaga spp. Rothia dentocariosa, Flavobacterium spp., Chromobacterium spp.
- Fungi: Yeasts are of primary concern
-- can cause fungemia (fungi inthe blood)
- Mycobacteria: Mycobacterium tuberculosis and Mycobacterium avium complex
- Brucella spp.
- Spirochetes: Borrelia spp., and Leptospira spp.
- Vitamin B6 - Dependent Streptococci: Granulicatella adiacens, and Abiotrophia defectivus
- Mycoplasma hominis
- Bartonella spp.: Bartonella bacilliformis, B. henselae, B. elizabethae, B. quintana
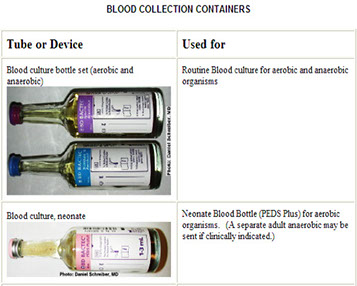
COLLECTION OF BLOOD SAMPLES
RECOMMENDATIONS
1. Any patient sufficiently ill to be hospitalized with a fever >100.4F or hypothermia (<96.8 F) or a leukocyte count of >10,000
2. In conjunction with urine and CSF in the evaluation of neonates with suspected septicemia
3. Children 2 and under with pneumococcal and Haemophilus influenzae bacteremia may present as outpatients with a marked fever and a high leukocyte count
4. Elderly may have nondescript complaints or even a low grade fever (may signal SBE)
SPECIMEN COLLECTION: SPECIFICS
1. Skin antiseptics/venipuncture
- Problem = contamination by microbial skin flora
- Endocarditis, especially on prosthetic heart valves, often caused by the same group of organisms normally found on skin
2. Anticoagulants
- SPS: Sodium polyanethol sulfonate
3. Volume
- 1-5ml; infants & children , 10ml; minimum for adults
4. Number of cultures/Timing
- Must consider the type of bacteremia (Transient, Intermittent, Continuous, etc.)
a) Suspected acute sepsis, meningitis, osteomyelitis, arthritis, or acute untreated bacterial pneumonia
- Two cultures from two different sites before therapy
b) Fever of Unknown Origin (FUO)
- Initially; Two seperate blood cultures, 24-36hrs. later get two more just before expected temperature elevation
c) Suspected Endocarditis
- Acute: Three cultures with three seperate venipunctures during first 1-2hrs. of evaluation
- Subacute: Three cultures on day one at least 15 minutes apart. If all negative at 24hrs., obtain three more
5. Culture Media/Additives
- Multipurpose nutritionally enriched liquid broth
- Two bottles normally inoculated (aerobic & anaerobic)
- Anticoagulant; SPS (0.025 - 0.05%) improves recovery by a variety of mechanisms
- 10 - 20% Sucrose; hypertonic sucrose broth
MISCELLANEOUS FACTORS IN BLOOD CULTURING
1. Dilution of Blood
- Normal dilution is 1:5 to 1:10
2. Neutralizing or Inactivating Antibiotics
- Blood cannot always be drawn prior to treatment
- Blood/broth dilution will also dilute antibiotic
- SPS inactivates aminoglycosides
- Penicillinase can be added
- Resins nonspecifically absorb antibiotics
3. Atmosphere of Incubation
- Commercial bottles have approx. 10% CO2 in air or an inert gas
- Aerobic bottle should be vented
- Anaerobic bottle should be under vacuum
4. Macroscopic Observations
- Turbidity, hemolysis, gas production, discrete colonins on sediment
- "Blind Subcultures" can be done
PROCESSING POSITIVE BLOOD CULTURES
- Type of growth often characteristic of certain organisms
- BacTec 9240 uses fluorogenic pH indicators to detect increased CO2 due to presence of microorganisms
- "Blind Subcultures" done only when Growth Index is positive but the Gram Stain = NOS
- Cultures routinely held for five days
- Positive Gram Stain results are called immediately to the floor
- Broth from Positive bottles is inoculated onto appropriate media
- Direct susceptibility testing can be done as well as some rapid biochemical tests.
- Final reports go out after five days incubation
- Lysis-Centrifugation can also be used
SPECIAL PROCEDURES
- Brucella spp, = Casteneda bottle
- Francisella spp. = Cystine + Glucose broth
- Leptospira = Fletcher's medium
- L-forms = Sucrose broth
- May use broth without SPS
MICROORGANISMS IN CEREBROSPINAL FLUID
3 syndromes caused by CNS infx: bacterial meningitis, viral (aseptic) meningitis, and encephalitis
- bacterial meningitis has inc WBC c neuts, dec gluc, MCC is GBS in neonates, Neisseria in kids and S pneumonia in adults
- aseptic meningitis has low WBCs c monocyte predominance inc protein and normal glucose, presents similar to bacterial meningitis, MCC is Enterovirus (7/10)
- encephalitis (Sx: MS changes) can give normal labs or those similar to aseptic meningitis
MENINGITIS
Sx: Fever, headache, stiff neck, nausea, vomiting, lethargy
Route of Infection - MC from blood, occasionally from a nearby focus
- Anatomic defects, surgically induced, congenital malformations
- Abcesses usually result from an embolism of bacteria or fungus from a distant site
AGENTS CAUSING MENINGITIS
- Agents include bacteria, mycobacteria, fungi, viruses, parasites
- MC bacterial & fungal agents are encapsulated
- MC bacterial agents are; S. pneumoniae, H. influenzae, N. meningitidis, Enterics, Listeria
- Agents vary with age and underlying disease
- lymphocytic choriomeningitis (LCM) MCC meningitis in winter; LCM infx causes problems in pregnancy
Neonates -from genital tract of mother
- E. coli, Group B Strep, Listeria
Infants & Children under 4 - Haemophilus influenzae type b
Older Children - Neisseria meningitidis and Streptococcus pneumoniae
Adults and Elderly - , S pneumo, Listeria or enterics
- Many adults are immunosuppressed or have had skull fractures
- Sepsis precedes most cases in the elderly
Immunodeficient and Immunosuppressed - Listeria frequently seen in patients with lymphoma and in patients on steroid therapy
- Leukopenic patients = Nocardia or Ps. aeruginosa
- Sickle cell, splenectomy, alcoholism, head trauma are predisposing factors for infection with S. pneumoniae
- Premature ruptured membranes = E. coli & Gp. B Strep (neonates)
- Brain abscesses usually caused by indigenous flora
- Patients with shunts = S. epidermidis, S. aureus, Corynebacterium spp., or Gram negative rods
- Cryptococcus neoformans in immunosuppressed patients
- Coccidioides immitis in endemic areas
- W Nile virus (Flavivirus) has bird reservoir and causes encephalitis c weakness paresis and neuropathy
- enteroviruses MCC of (viral) aseptic meningitis
SPECIMEN COLLECTION
CSF is collected by aseptically inserting a needle into the subarachnoid space at the level of the lumbar spine
- Need as much as possible
- CSF in Micro is centrifuged, stained, and cultured onto media
- Brain abcesses: need aspirate, NO SWABS, and transport media for anaerobic culture
MICROSCOPIC EXAMINATION
- Gram stain; may use basic fuchsin as counterstain
- Fluorescent Staining --> Acridine Orange
- India Ink --> Cryptococcus
- Acid Fast stain --> Mycobacteria
CULTURING CSF
- Sediment is inoculated onto BAP/CHOC/Thio
- Incubate under CO2 at 35"C
- Abscesses: BAP/CHOC as well as anaerobic media
NON-CULTURE METHODS
- Limulus Amoebocyte Lysate (LAL) detects Gram negative endotoxin
- CIE detects bacterial antigens in body fluids
- Coagglutination and Latex Agglutination now widely used (rapid and simple to perform)
- ELISA : variety of tests available, usually done in microdilution trays and read on a plate reader
- GLC can be used to detect metabolic products of various organisms in CSF
- Latex agglutination can be done on SHiN bacteria and GBS
REPORTING RESULTS
- All positive results must be reported immediately
- Patient history can be a key to early diagnosis
CEREBROSPINAL MENINGITIS EPIDEMICS
- Epidemics of meningitis seen in developing countries especially across central Africa
- Almost always caused by Neisseria meningitidis serogroup A
Sx: Extremely rapid onset; fever, malaise, severe headache, neck rigidity, aversion to bright lights
- Often fatal if untreated due to coma and shock
- Inflammation of the meninges causes a profound septic shock resulting in loss of blood pressure
- Patients who survive may suffer a disfiguring loss of skin and parts of limbs
- Deafness, paralysis, and mental retardation may also result
EPIDEMIOLOGY - Climate, an immunologically susceptible population, a specific serogroup of N. meningitidis, and viral respiratory tract infections all play a role in outbreaks
- Neisseria lactamica and Mycoplasma hominis may also be factors to consider
- Enzyme electrophoresis has been used to delineate at least 21 clones of serogroup A and clone III-1 has recently caused epidemics in Africa, Asia, and the Middle East
- Antigenic shifts similar to that seen with influenza may occur with N. meningitidis serogroup A
- Intervals of five to twelve years are observed between epidemicsof meningitis in Central Africa

Ear and Eye Infx
EAR INFECTIONS
OTITIS MEDIA
● Acute & chronic inflammation of the middle ear
● Acute form seen primarily in infants and children
● Most infections are bacterial and accompany or follow viral infection
1. Children
● 50% Streptococcus pneumoniae
● 20-30% Haemophilus influenzae
● 10-20% Streptococcus pyogenes
2. Adults
● >90% Streptococcus pneumoniae
● also; Gp.A Strep, Staphylococcus aureus, H. influenzae
● chronic otitis media with discharge is usually caused by: Pseudomonas, Proteus, E. coli
● S. aureus & Ps. aeurginosa MC in tx failures
OTITIS EXTERNA
● Inflammation of the external auditory canal
● Predisposing factors; high humidity & temperature, allergy to hair spray
● In chronic cases Pseudomonas becomes predominant, then S. aureus
● Acute localized disease (pustule or furuncle) ; usually S. aureus
● Erysipelas due to Streptococcus pyogenes
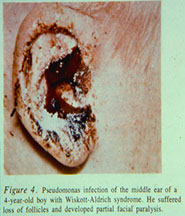
MALIGNANT OTITIS EXTERNA
● Infection beginning in external auditory canal and extending into the temporal bone
● Seen primarily in elderly diabetics & patients with blood disorders
● Facial nerve paralysis may result
● Caused by Pseudomonas aeruginosa
EYE INFECTIONS
INTRODUCTION
● Techniques for microbiologic investigation are determined by site of infection, severity of infection, and knowledge of likely responsible microorganisms.
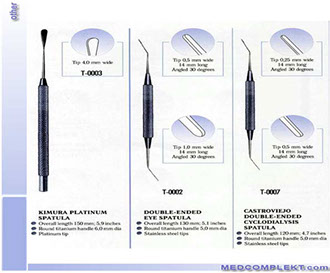
SPECIMEN COLLECTION
● Use Kimura Spatula to collect material from conjunctiva & cornea
● Swabs: cotton, polyester, calcium alginate are acceptable
● Swabs must be transported in transport media
● Needle & syringe aspirate for anaerobes or commercial anaerobic transport media
● Include media appropriate for Haemophilus & Neisseria, Anaerobes, Fungi, and Mycobacteria
BACTERIAL EYE INFECTIONS
Conjunctivitis
● Usual flora: S. epidermidis, S. aureus, Corynebacterium spp. others
● Routes of inoculation: airborne, hand to eye, spread from adjacent areas
● Endogenous conjunctivitis is uncommon
● Clinical presentation & history often suggests causative agent
● Acute Bacterial Conjunctivitis is characterized by edema of eyelids and a purulent discharge
● Common agents include; S. aureus, Gp.A Strep, S. pneumoniae, H. influenzae, N. gonorrhoeae, M. lacunata (pinkeye), C. diphtheriae
Neonatal Conjunctivitis
● Infection occurs by three primary routes
A. Ascending infection from vagina & cervix
B. Inoculation by genitourinary secretions at birth
C. Contact with contaminated materials or persons during the neonatal period
● Clinical signs do not suggest causative agent
● Common agents include; Chlamydia, N. gonorrhoeae, S.aureus, Streptococcus pyogenes
● Ps. aeruginosa is a rare but potentially fatal infection in premature infants
Orbital Cellulitis
● Acute inflammation of orbital tissues
● Routes of inoculation
A. inoculation by trauma or surgery
B. extension of infection from other structures
C. spread from sinus infection
● H. influenzae MCC in children <5yrs.
● Adults; S. aureus, Gp.A Strep, S. pneumoniae, Ps. aeruginosa
● Blood cultures usually positive in children with orbital cellulitis when caused by H. influenzae
● Aspiration of the orbital abcess is NOT recommended
Eyelids, Lacrimal Gland, Lacrimal Ducts, and Lacrimal Sac
● Infection results in interruption of function
● Chronic infection may result in permanent loss of function
● A "sty" is an example of infection in this area (caused by Staphylococcus aureus)
Bacterial Corneal Ulcers
● Bacterial ulcers occur following trauma to the cornea
● When colonization occurs, an abcess is formed which progresses to an ulcerative process
● Contaminated ocular solutions, contact lenses
● Spontaneous infection caused only by bacteria capable of epithelial colonization and penetration
● Organisms include; N. gonorrhoeae, C. diphtheriae, and H. aegypticus
● Scrapings must be carefully examined as very few organisms may be recovered
● Following trauma, most common causes of bacterial corneal ulcers include; S. pneumoniae, S. aureus, Ps. aeruginosa, and Moraxella spp.
Endophthalmitis
● Inflammation involving the interior of the eye
● Most serious and sight-threatening of occular infections
● Exogenous infections usually follow intraocular surgery
● S. aureus is most common agent following cataract surgery
● Bacillus sp. causes most severe & rapidly progressive form of exogenous endophthalmitis
● Endogenous infection occurs as complication of sepsis, usually in compromised hosts or drug addicts
● Agents include; Cryptococcus sp., Candida sp., S. aureus, S. pneumoniae, N. meningitis, Mycobacterium sp., and Bacillus
● Lab diagnosis requires collection of intraoccular fluid
OTHER EYE INFECTIONS
Viral Infections
● Herpes simplex, Varicella zoster, Adenovirus
Fungal Infections
● Mycotic keratitis
● Caused by numerous fungi but over half of all cases caused by Fusarium solani
● Others include; Aspergillus, Acremonium, Curvularia, and others
Chlamydial Infections
● Endemic or Classic Trachoma
● Inclusion Conjunctivitis
SINUS INFECTIONS
ANATOMY
● The mastoid is a portion of the temporal bone containing the mastoid sinuses
● Mastoiditis is often a complication of chronic otitis media
● The sinuses are unique air-filled cavities within the head that are lined by respiratory epithelium
● The sinuses are normally sterile
DISEASES
Acute sinusitis
● Acute sinusitis usually develops during a cold or influenza-type illness
● Purulent nasal and postnasal discharge, pressure over the sinus areas of the face, cough, nasal quality to voice, fever
● Usually lasts one to three weeks, tends to be self-limited
Chronic sinusitis
● Bacterial colonization occurs and fails to respond to antibiotic treatment
● Surgery or drainage is required for effective treatment
● Acute exacerbations may occur
● Complications: local extension into the orbit, skull, meninges, brain
PATHOGENESIS AND EPIDEMIOLOGY
● Most cases are bacterial complications of viral colds
● 5-10% of maxillary sinus infections result from a dental source
● Chronic sinusitis is associated with inadequate drainage, impaired mucocilliary clearance, mucosal damage
● Most cases occur from the fall through spring seasons
● Bacterial cultures are positive in 3/4 of cases of maxillary sinusitis
● Agents include: H. Influenzae 50%, St. pneumoniae 19%. Also St. pyogenes, M. catarrhalis, P. acnes, and other skin flora
● With children: St. pneumoniae, H. influenzae, and M. catarrhalis
LABORATORY DIAGNOSIS
● Diagnosis can often be made on physical findings, history, radiograph studies and other imaging techniques
● Sinus drainage is unacceptable for culture due to contamination with normal respiratory flora
● Material for culture is obtained by puncture and aspiration of the maxillary sinus
● Specimens are Gram-stained and set up for aerobic and anaerobic culture (for aerobic culture: BAP. Choc, and Mac)

Otitis externa

Malignant otitis externa
Eye spatulas

Neonatal conjunctivitis

Orbital cellulitis

Sty
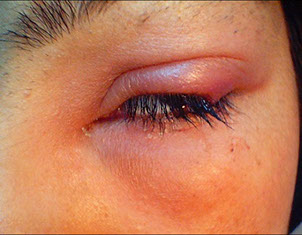
Chlamydial eye infection



Genital Tract Infections
INTRODUCTION
Usual flora of the genital tract consists of Enterics, anaerobes, various Streptococcus spp., Lactobacillus, Staphylococcus and Corynebacterium spp.; also Group B Streptococcus.
NON-VENEREAL INFECTIONS
GENERAL
● Non-venereal infection of the female genital tract are of two types: 1. Pyogenic and 2. Granulomatous
● These occur as 1. Exogenous or 2. Endogenous
PYOGENIC
● Originate in poorly oxygenated, poorly defended spaces that contain substances that promote rapid bacterial growth.
● Examples;
1. Septic Abortion: Infection frequently follows an induced incomplete abortion
● Bacteremia occurs in over 50% of cases
● Most patients recover but when complications occur they are severe.
2. Post-Partum Endometritis: Usually begins 2-5 days after delivery
● Lacerations of cervix & uterine wall predispose to infection
● Majority of infections caused by endogenous bacteria (E.coli and anaerobes. Also; S. aureus, N. gonorrhoeae, and S. pneumoniae )
GRANULOMATOUS
● Primarily caused by Mycobacterium tuberculosis
● Rarely can be caused by Histoplasma capsulatum or Coccidioides immitis
● M. tuberculosis reaches the fallopian tubes via the blood and can move upward to produce pelvic peritonitis or downward to produce endometritis
VAGINITIS
● Abnormal increase in vaginal secretions
● Purulent discharge caused by N. gonorrhoeae, I.U.D.'s, or possibly Chlamydia
● Other conditions/causes
1. Trichomonas vaginalis: Infection usually clears with treatment
● Lab Diagnosis: Wet mount (sometimes culture)
2. Candida albicans: Present in feces
● Altered host resistance plays important role
● Vulvovaginitis
● Lab Diagnosis: Gram stain & Culture
3. Bacterial vaginosis: Most often attributed to Gardnerella vaginalis
● Most cases are polymicrobic and involve other organisms besides G. vaginalis (anaerobes, particularly Mobiluncus)
● Sexually active females more prone to infection
● Lab Diagnosis: HBT agar, biochemical tests, "clue cells"
TOXIC SHOCK SYNDROME
● Acute febrile illness
● Menstral period + tampon use + Staphylococcus aureus toxin
● Two suspect toxins; (collectively referred to as TSST-1)
1. Type C , heat labile
2. Type F , heat stable
● Recurrent infections are common (about 40%)
Sx: Fever, sore throat & mouth, headache, weakness, body aches, conjunctivitis, vomiting, abdominal pain, watery diarrhea, rash.
● May become disoriented and lose consciousness
● Shock, renal and respiratory failure may occur
● Desquamation of skin and hair loss
CDC Criteria for Toxic Shock Syndrome
1. Fever over 102○F
2. Rash + Desquamation of skin
3. Hypotension
4. Involvement of three or more organ systems. (G.I.,
muscular, mucous membranes, renal, hepatic, CNS, hematologic)
5. Negative cultures of blood, CSF, and throat and negative serological tests.
SEXUALLY TRANSMITTED DISEASES
GONORRHEA
● Neisseria gonorrhoeae is the etiologic agent
● Cervicitis in women............Urethritis in men
● Can spread by ascending route in genital tract or via blood
● Gonococci can also infect other mucous membranes
● Individuals w/o symptoms may be colonized & infect others
● Men: Incubation period 2-5 days;
● Typically painful urination with purulent discharge
● Most men are symptomatic (some carriers exist)
● Sterility is major complication.
● Women:
● Most women are asymptomatic
● Primary site = cervix, Secondary site = urethra & rectum
● Gonococci may ascend to infect fallopian tubes and the pelvic area producing Pelvic Inflammatory Disease (PID).
● Neisseria meningitidis can be isolated from the same sources
NONGONOCOCCAL URETHRITIS
● Usually less severe than gonorrhea
● May co-exist with gonorrhea and become evident after treatment for G.C.
● Chlamydia trachomatis causes at least 50% of cases
● Other Causes; Mycoplasma, Trichomonas, Herpes, perhaps Candida
● In men there is a 20-30% incidence of asymptomatic Chlamydial infection when gonorrhea has been treated.
● In women the Chlamydial infection is usually asymptomatic but may play a role in PID.
● 50% of women with cervical gonorrhea also have a Chlamydial infection = "female urethral syndrome"
SYPHILIS
● Etiologic Agent = Treponema pallidum
● Aquired by direct sexual contact
● Ulcerated papule at initial site = primary "chancre".
● Dissemination from primary site results in widespread cutaneous lesions = secondary syphilis
● Lesions resolve spontaneously but relapses occur in 20% of patients (leading to tertiary syphilis)
● Gumma - are characteristic of tertiary syphilis
● Genital lesions must be differentiated from Herpes
● Lab Diagnosis:
● Darkfield exam in early syphilis
● Presence of Ab to cardiolipin (VDRL or RPR)
● Presence of Ab to Treponemal Ag (FTA-ABS, TPI)
GENITAL HERPES
● Acute inflammatory infection of males and females
● Etiologic agent is Herpes simplex type 2
● Recognized as STD in the 1960's
● Divided into primary (venereal exogenous infection) and recurrent infections resulting from recurrent endogenous Herpes
● Incubation period 2-20 days
● Primary infection more severe and prolonged (painful lesions)
● Usually self-limiting w/o complications
● Exceptions: Immunosuppressed, Compromised, Pregnancy
● Lab Diagnosis: FA Staining, Isolation in tissue culture
CHANCROID
● Etiologic agent is Haemophilus ducreyi
● Shallow genital ulcers, enlarged lymph nodes
● Also referred to a "Soft Chancre".
● Highly contagious, major public health problem in the tropics
● Incidence increases in wartime (association with prostitutes)
● Recent large outbreaks in Canada & Orange Co. Calif.
- Lab Diagnosis: Gram stain ulcer or lymph node exudate, culture on chocolate agar + isovitalex + hemoglobin + vancomycin or on rabbit blood + isovitalex + vancomycin ( 33-35○C under CO2)
GRANULOMA INGUINALE
● Rarest of STD's in Europe and North America
● Endemic in tropical and subtropical climates
● Slowly progressive cutaneous ulceration
● Klebsiella granulomatis is the etiologic agent
(Cannot culture on artificial media / cultured in embryonated eggs)
● Encapsulated plump bipolar Gram negative bacillus
● Has been isolated from feces (may be a fecal reservoir)
● If treated early it is benign with no complications
● Untreated may lead to extensive tissue destruction with sepsis and
death due to bacterial infection.
● Lab Diagnosis: Wright's or Giemsa stain of ulcer scrapings to confirm presence of Donovan Bodies.
● Donovan Bodies: Large mononuclear cells will have intracellular pleomorphic blue to purple rods surrounded by pink capsules.
LYMPHOGRANULOMA VENEREUM
● Caused by Chlamydia trachomatis
● World-wide distribution but endemic in tropical climates
● Primary lesion appears in 2-4 wks.
● Organism transported to the lymph nodes
● Most patients recover w/o complications
● Lab Diagnosis: Direct FA stains, culture and serological testing
CONDYLOMA ACUMINATUM
● Genital Warts or Venereal Warts
● A contagious projecting warty growth on the external genitals or anus
● Consists of fibrous overgrowths covered by thickened epithelium
● Usually benign
● Caused by human papilloma virus
OTHER SEXUALLY TRANSMITTED AGENTS
● Trichomonas vaginalis ● Gardnerella vaginalis
● Shigella spp. ● Campylobacter spp
● Salmonella spp.


Clue cells, G vaginalis


T pallidum

Secondary syphilis
Tertiary syphilis

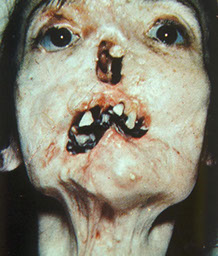
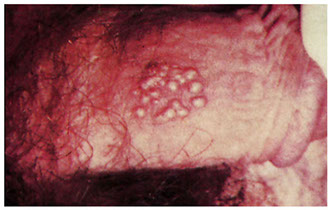
Chancroid

Granuloma inguinale

Donovan bodies
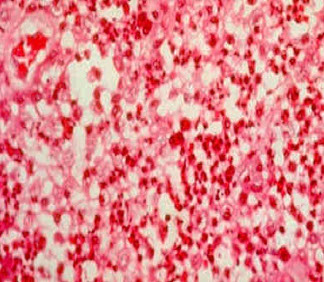
Condyloma acuminatum

Gastrointestinal Tract Infections
INTRODUCTION
● Potential pathogen ingested --> attachment to mucosal epithelial cells in specific areas of G.I. tract
● Bacterial surface structures necessary for bowel colonization
- MCC acute infx diarrhea is viral (1/2), esp norovirus, enteric adenovirus and rotavirus
- then E coli + other bacteria (more prolonged dz, bloody possibly if inflammatory), protozoa least comn
-- bloody diarrhea w/o fecal neutros = EHEC 0157:H7
-- travelers get ETEC
-- C diff after hospitalization, possibly elderly after abx
MECHANISMS OF PATHOGENICITY
A. Attachment w/o penetration- enterotoxin production
● Cytotoxins & neurotoxins can also be involved
B. Adherence to microvilli w/o penetration
C. Attachment, penetration, multiplication within epithelial cells
D. Attachment, penetration, multiplication within submucosa
CLINICAL ASPECTS
● Diarrheal illness varies from mild to severe
● Clinical presentation often not helpful in suggesting etiologic agent
A. Small bowel infection with non-invasive agent
● Enterotoxin produced; voluminous diarrhea, no blood or leukocytes, no significant fever
● Marked dehydration
B. Large bowel infection with invasive agent
● Pathogenicity due to invasive properties
● Frequent diarrheal stools of small quantity
● Blood and pus cells present, abdominal pain, fever
● Relatively mild dehydration
C. Gastritis
● Nausea, upper abdominal pain, vomiting, burping, fever
● Etiologic agent --> Helicobacter pylori
D. Treatment
● Replacement of fluid & electrolytes will correct dehydration
● Antimicrobial therapy indicated only under specific conditions (ie. cholera or severe shigellosis)
● Treatment of gastritis is more specific
LABORATORY ASPECTS
A. Specimen Collection and Transport
● Feces, duodenal contents, vomitus
● Rectal swabs when feces are not readily available
● All specimens should be cultured ASAP
● Transport medium used if delay of >2hrs. is anticipated (phosphate buffered glycerol, Carey-Blair)
● 1gm feces/10ml medium
● Fecal leukocytes sometimes helpful
B. Processing of Specimens
1. Routine Cultures
● BAP (recommendations vary)
a) Enteric Agars
● Differential: MAC, EMB
● Moderately Selective: HE, XLD, SS
● Highly Selective: BG, BS
b) Enrichment Broth
● GN, Selenite F, Tetrathionate
c) Campylobacter Media
● Skirrow's, Blaser's, Butzler's, Preston's
● Growth Requirements: microaerophilic atmosphere, 42 C
● Enrichment Techniques: Campy-Thio
2. Special Culture Techniques
a) Aeromonas : BAP-AMP, MAC or EMB, BAP
b) Plesiomonas : Inositol-Brilliant Green-Bile Salts agar, BAP, MAC, HE
c) Vibrio spp.: TCBS, alkaline peptone water
d) Yersinia spp.: CIN/250C, cold enrichment ?, alkalai treatment (KOH)
e) Clostridium difficile: CCFA, toxin testing
f) Hemorrhagic E. coli (E.coli O157:H7): sorbitol-MAC to work up or send to reference laboratory
g) Escherichia coli (usual isolates): no special media required, select five colonies to work up
h) Miscellaneous bacterial agents: Bacillus cereus, Clostridium perfringens, Clostridium botulinum, Staphylococcus aureus
i) Culture not usually attempted for H. Pylori
3. Preliminary Identification Procedures
● Stool Screen: TSI, LIA, URE
● Conventional biochemical tests
4. Confirmatory Identification Procedures
● Automated Identification Systems (ie. Vitek)
● Rapid Identification Kits (API)
● Bacterial Serology (Salmonella & Shigella)
BACTERIAL AGENTS OF DIARRHEAL DISEASE
A. Enterotoxigenic Species
1. Vibrionaceae
● V. cholerae O:1 & other Vibrio spp. (cytotoxins also)
● Aeromonas and Plesiomonas
2. Clostridium difficile
● Enterotoxin and cytotoxin production
3. Agents related to food poisoning
● Staphylococcus aureus
● Bacillus cereus
● Clostridium perfringens
● Clostridium botulinum
4. Escherichia coli
● ETEC
● Enterohemorrhagic E. coli O157:H7 (cytotoxins also)
● SLTEC Shiga-like toxin-producing E. coli O104:H21
B. Enteroinvasive Species
1. Salmonella spp.
● S. Typhi: penetration of submucosa
2. Shigella spp.
● S. Dysenteriaeae: cytotoxin also
3. Escherichia coli → EIEC (enteroinvasive E. coli)
4. Yersinia enterocolitica
● Penetration of submucosa tissue
5. Campylobacter jejuni & Campylobacter coli
● Cytotoxin also
6. Miscellaneous invasive bacterial species
C. Neurotoxin activity
● Clostridium botulinum
D. Non-Invasive, Non-Toxigenic bacterial species
● Escherichia coli : EAEC and EPEC


Mech of Cholera


Heart
Infective endocarditis
Ddx depends on the valve, consider as 3 different syndromes: infx of a previously normal valve, infx of an abnormal native valve, and infx of prosthetic valve
- should get 3 sets of 2 cultures over 24 hr (q8h)
- Gram stain of an excised valve can be misleading as abx tx can alter stained organism morphology
Infx of previously normal valve
2/2 very virulent orgs that destroy the valve
- MCC: S aureus, S milleri also popular
- S auerus causing tricuspid endocarditis in IVDU
- Austrian's syndrome - endocarditis, meningitis and pneumonia, endocarditis seen in alcoholics c pneumococcal endocarditis, not seen much anymore
Infx of an abnormal native valve
2/2 less virulent organisms that tend to form vegetation but do not destroy valve, causing subacute bacterial endocarditis (SBE)
- MCC: Viridans strep, grp B strep, grp D strep, Enterococci, and other HACEK bugs
- abnormality usually 2/2 rheumatic heart dz on mitral
- sx 2/2 the infx: valve dysfunction (hemodynamic instability), vegetation emboli (Roth spots, stroke, kidney damage, Osler nodes), immune stim (rheumatoid factor, immune complexes)
Infx of prosthetic valve
2/2 S epidermidis and S aureus
- involved in the valve suture ring, causing stenosis, dehiscence, and dysrhythmia
Blood Culture Negative Endocarditis (BCNE)
Assoc c prior abx use, assoc c Coxiella burnetti, Bartonella, Chlamydia and Legionella
- must also r/o non-infective endocarditis like Libman-Sacks, marantic and carcinoid heart syndrome
Respiratory Tract Infections
UPPER RESPIRATORY TRACT (URT)
● consists of the nasopharyngeal region, the oropharyngeal region and the pharynx
● The larynx connects the pharynx to the lower respiratory tract
● Most infections are self-limiting and are caused by viruses or Mycoplasma
● The biggest problem is to identify a pathogenic or potentially pathogenic bacterium from a large number and variety of indigenous bacterial flora
● Some potential pathogens are simply part of a carrier state
USUAL FLORA
● The oropharynx has a dense bacterial population
● Anterior nares are colonized (S. epidermidis & Corynebacterium spp.)
● The sinuses and the lower respiratory tract do not have a resident bacterial flora in healthy individuals
PHARYNGITIS
● Primary cause in North America = Streptococcus pyogenes
● Less commonly; C. diphtheriae and Candida albicans
● Predominance of H. influenzae type b in children may be significant
● Streptococcus Gps. C & G as well as some Corynebacterium spp.have also been implicated
● Pure cultures of S. pneumoniae or Staphylococcus are usually indicative of viral pharyngitis
● Pure culture of Ps. aeruginosa often seen when patient is on antimicrobial therapy
● URT of hospitalized patients frequently colonized by Pseudomonas, Kl. pneumoniae, and other enterics
● Routine screening for meningococcal or gonococcal pharyngitis is not normally done.
Streptococcal pharyngitis
a. Specimen of Choice: good throat swab
- Direct Smears: not recommended
- Cultures: BAP c sheep blood
d. Presumptive Identification: B-hemolytic colonies on Taxo A disk
e. Confirmatory Identification: serology MC, or latex coagglutination
f. Susceptibility Testing: not practical as GAS universally susceptible to penicillin
Gonococcal Pharyngitis
● Confirmatory testing is required
- direct antigen testing used in outpt setting
3. Reporting Results - Reports must include which organisms were looked for, what was found, and a quantitative evaluation
LARYNGITIS AND EPIGLOTTITIS
● Acute laryngitis is almost always viral (diphtheria might be a rare exception)
● Epiglottitis is uncommon but can be life threatening
● Infections of the epiglottis are primarily bacterial, usually seen in children, and normally caused by H. influenzae type b
● Diagnosis of epiglottitis is essentially a clinical one. Swabbing for culture is not recommended
SINUSITIS
● Sinuses are vulnerable to infection by URT organisms
● Acute sinus infections are often precipitated by viral infection
● Other factors include allergies, deviated septum, polyps
● All of the above may contribute to obstruction of the sinus openings, impeding drainage and encouraging colonization
● Infections may become chronic or may spread to other tissues with possible
complications: Brain abscess, meningitis, etc.
● Common organisms = S. pneumoniae, Staphylococcus, Streptococcus, Klebsiella spp., Bacteroides, and occasionally H. influenzae
● Anaerobes may play prominent role in chronic cases
NASOPHARYNX AND NASAL
● Nasopharyngeal cultures usually ordered with the following;
1. Sepsis workup of neonates
2. Detection of carriers
3. Diagnosis of Diphtheria & Perutssis
4. Acute sinusitis and Otitis media workup in children
MISCELLANEOUS INFECTIONS OF URT
1. Thrush
● Yeast infection caused by Candida albicans
● Common in neonates & debilitated adults after treatment with broad spectrum antibiotics
(also in AIDS patients)
● Lab diagnosis: Gram stain or KOH prep of exudate
2. Vincent's Angina
● Rare ulcerative infection of gums, mouth, or throat (adults)
● Poor oral hygiene or serious systemic disease predispose
● Caused by certain anaerobes (F. necrophorum) and a spirochete (B. vincentii)
● Lab diagnosis: Gram stain (carbol fuchsin), cultures are of no diagnostic value
LOWER RESPIRATORY TRACT
● Organisms responsible for infection often suggested by clinical presentation, age of patient, underlying disease, travel history, and occupation
● Other important factors: was infection nosocomially acquired? and is patient receiving treatment or antimicrobial therapy?
MCC community-aq pneumonia in health adults: Mycoplasma pneumonia, Chlamydia pneumonia, Strep pneumonia, Hemophilus pneumonia
- old ppl in nursing homes: S pneumonia, H influenza, aerobic gram-neg bacilli
- ventilator pts: S aureus, S pneumonia, P aeruginosa, K pneumonia, Serratia, Enterobacter, fungi, E coli
- COPD: H influenza, M atarrhalis, Legionella p
- Alcoholics: S pneumonia, anaerobes (aspirated), gram neg aerobic bacilli
- Neutropenics: aerobic gram neg bacilli
- Sandstorms - coccidiomycosis
- Bronchiectasis / Cystic Fibrosis - P aeruginosa, Peudomonas cepacia, S aureus
- SARS (Severe acute respiratory syndrome) comes from China and caused by Coronavirus, (collectively called SARS-CoV) producing flu resembling DAD
SPECIMEN TYPES AND COLLECTION
● Interpretation of results depends on specimen source and organisms recovered
● Some organisms are implicated as pathogens regardless of source
● Some organisms are difficult to recover and require special techniques
● Some specimens are more likely to become contaminated with URT flora than others
● Interpretation based on microscopic appearance, semi-quantitative results, and clinical correlation
MICROSCOPIC EXAMINATION
1. Gram Stains
● Performed on all sputum specimens
● Specimens evaluated by # of eptihelial cells and # of leukocytes per low power field
● Ideally <10 epithelial cells & >25 leukocytes /lpf
2. Examination for Mycobacteria
● Specimens must be decontaminated and concentrated
● Smears are prepared and Acid-Fast stains are performed (FA and classical ZN stains)
● Results of smears are reported semiquantitatively (#organisms per field)
3. Wet Unstained Preparations
● Used primarily for fungi
● Specimen is mixed on slide with KOH and glycerol
- KOH clears epithelial cells and allows visualization of fungal elements
D. CULTURING
1. General
● The best collection techniques bypass the usual flora of the URT
● Goal is to process specimens in a manner that maximizes the isolation of the more common pathogens
2. Processing
● Generally the most purulent portion is selected
● Media: BAP, CHOC, and a differential medium
3. Examination
● Plates are examined after overnight incubation
● Sputum: only predominant growth should be identified & reported
● Aspirates: all colony types identified and reported
- pts c tracheostomies unable to produce sputum in normal manner, so lower respiratory secretions collected in Leukens trap, and treated by lab as sputum
4. Minimal recommendation for Identification
● Streptococcus: differentiate between S. pneumoniae and other α-hemolytic Strep, and Gp. A Strep from other β-hemolytic Strep
● Staphylococcus: must separate S. aureus from other Staph
● Neisseria: identification to species not normally necessary
● Gram positive rods: no need to identify to species (most are Corynebacterium spp.)
● Enterics: should be identified if predominant, particularly in debilitated and hospitalized patients
● Non-Fermenters: should be able to identify Ps. aeruginosa
● Special Procedures: special media and techniques required to isolate and identify the
following LRT pathogens; Mycobacteria, Nocardia, Bordetella, Legionella, Mycoplasma, as well as the various fungal pathogens

Thrush

Vincent's angina

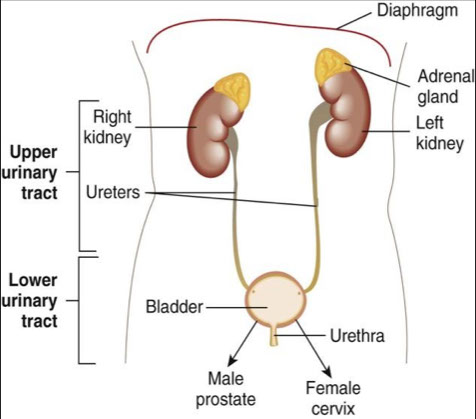
Urinary Tract Infections
● UTIs one of the MC bacterial diseases
● Affects all ages, both sexes, mild or systemic
● Affects the kidneys, ureters, bladder, and urethra
● Most result from an ascending infection
● Acute infections more common in females (except neonates, similar freq in M/F >50 yo)
● Urine is an excellent culture medium
● Value of quantitative testing has been established
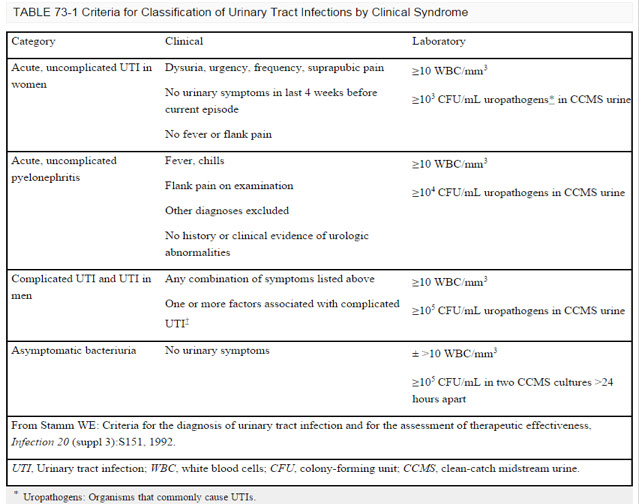
● Counts of 10^3 (1000) organisms/ml is dx of cystitis per IDSA
Exceptions: patients on antimicrobial therapy
patients excessively hydrated
presence of fastidious organisms
infants and children
urinary obstructions
CLINICAL CONDITIONS
Sites
● Urethra: urethritis ● Bladder: cystitis
● Prostrate: prostatitis ● Kidney: pyelonephritis
Urinary tract infections in women
- preg women c asx bacteriuria need tx
● Most common sites = urethra and bladder (urethrocystitis)
● Enterics responsible for almost all nongonococcal urethrocystitis
● Escherichia coli responsible for ~90% of all cases
● Others: Klebsiella spp., Proteus spp., Pseudomonas spp., Enterococcus spp., Acinetobacter spp., Alcaligenes spp. etc.
● Candida albicans may also be involved in UTI's
● Staphylococcus saprophyticus considered a major pathogen in sexually active young women
● Staphylococcus aureus occasionally causes cystitis
● Other possibilities: Chlamydia, Mycoplasma, Gardnerella vaginalis
Urinary tract infections in men
● Major problem: chronic infections of the prostrate
● Usually caused by Gram negative rods....Escherichia coli (80%) , Klebsiella spp., Proteus spp., Pseudomonas spp., Enterobacter sp.
● 10% of men have polymicrobic infections
● Enterococcus spp. may occasionally be a problem
- Hemorrhagic cystitis in BM transplant pts caused by adenovirus
- culture negative UTI - think CUM, Chlamydia, Ueaplasma and Mycoplasma hominis
Pyelonephritis
● Inflam that involves both the pelvis and the kidney
● May lead to renal destruction
● Bacteria infect the kidney by ascending via the urethra or by the blood stream
● Usually caused by Escherichia coli (90%) also other enterics, some Enterococci and rarely Staphylococcus spp.
SPECIMEN COLLECTION
COLLECTION AND TRANSPORT
● Collection, storage, and transporting specimens are critical
● Contaminating bacteria can invalidate the tests
● If specimens are not examined or cultured within one hour they must be refrigerated.
- dipstick for hemoglobin sensitive, not spec for UTI
- leukocyte esterase >sens than dipstick, but not spec
- dipstick nitrite spec, but not sens
- eosinophiluria = Acute Intestitial Nephritis, not UTI
TECHNIQUES
1. Diagnostic catheterization
● Once considered best method of collection
● Definite risk of introducing infection
2. Clean Voided Midstream
● Must be quantitative (105/ml)
● Recommended in most cases
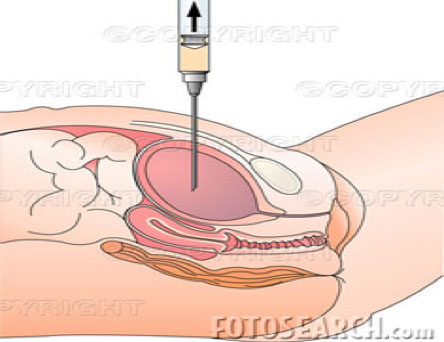
3. Suprapubic aspiration
● Occasionally necessary to verify infection
● Helpful with small children & adults with questionable results
● Specimens are likely to be sterile
4. Indwelling catheter
● Urine should not be collected from drainage bag
● Needle aspirate of catheter preferred collection method
● Culture of catheter tip is not recommended
RECOMMENDED BASIC PROCEDURE
TIMING
● Obtain early morning specimen when possible
OBTAIN A CLEAN VOIDED SPECIMEN
INFORMATION REQUIRED
● Clinical diagnosis, method of collection, time collected
● Antimicrobial therapy, fluids given
HANDLING OF SPECIMEN
● Should be processed immediately or refrigerated
● Specimens more than one hour old without refrigeration should be rejected by the laboratory
EXAMINATION
MICROSCOPIC EXAMINATION
● Gram Stain of uncentrifuged urine is considered useful and good screening technique
● 10^5 organisms/ml = one or more orgs per field
● Many epithelial cells + few pus cells + mixed flora is indicative of contamination
QUANTITATIVE COLONY COUNTS
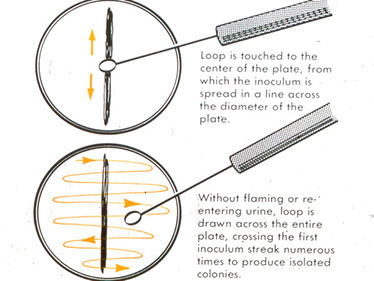
1. Surface Streak Procedure
a) Calibrated Loop Technique
● Loops are calibrated to deliver 0.001mL or 0.01mL
● One loopful of urine is streaked onto the plates
b) Pipette Technique
● 1/100 dilution of urine is made in distilled water
● 0.1mL inoculated onto surface of plate and spread evenly
2. Pour Plate Technique
● Mix 0.1mL or urine with 9.9mL of distilled water
● Pipette 0.1mL of diluted urine into empty petri dish
● Add 10-20mL of clear medium
CULTURING
● Media used include: EMB or MAC, and a BAP
REPORTING
1. Less than 10 colonies = probably a contaminant
2. 10-100 colonies = report number of organisms/mL urine
● If a single organism predominates, it should be identified
● If a mixture of two or more organisms report as mixed flora
3. 100 or more colonies = report as greater than 10^5/mL
● If more than one colony type; Identify all
● If more than two species are found; suspect contamination
SPECIAL SITUATIONS
SUPRAPUBIC / CYSTOSCOPY SPECIMENS
● These specimens are not likely to be contaminated
● Recommended that additional plates be inoculated
SEROTYPING / BIOTYPING
● Can be helpful in differentiating between recurrent infections and new infections
● Relapses may be due to inadequate therapy
SCREENING
● Gram Stain
● Leukocyte esterase & nitrate test
● Instrumentation (lumac & others)
ACUTE URETHRAL SYNDROME (AUS)
● Females with symptoms of lower UTI (Bladder) and pyuria but with counts of less than 10^5
● As many as 1/3 of all women who seek attention for complaints and symptoms of acute cystitis may fall into this group
● A cutoff of 10^2 is recommended but there must also be concommitant pyuria
● Most common agents: Escherichia coli, Klebsiella, Enterobacter, Staphylococcus saprophyticus
● Treatment depends on the etiologic agent
● Patients with sterile pyuria → Chlamydia or gonorrhoeae (genital Mycoplasmas or Herpes may also be involved)


calibrated loop
References
1.
